Imagine treating breast cancer without a single incision, without a scar, and without the fear of going under the knife. What once sounded like a distant dream is now becoming a medical reality — and for millions of women in Pakistan, it could not have come at a better time.
A non-invasive treatment known as High-Intensity Focused Ultrasound, or HIFU, is drawing serious attention from oncologists and cancer researchers worldwide, including in South Asia, for its ability to destroy breast tumours using precisely targeted sound waves — entirely from outside the body. As Pakistan continues to battle one of the highest breast cancer rates in Asia, specialists say this technology may open a door that conventional treatment has long kept half-shut for many Pakistani women.
What Is HIFU and How Does It Actually Work?

HIFU — short for High-Intensity Focused Ultrasound — is not your regular diagnostic ultrasound. While the kind used in hospitals to see inside the body is gentle and passive, HIFU uses high-frequency sound waves focused into a tiny, precise point inside the tumour tissue.
When those sound waves converge on the target, they generate intense heat — temperatures can rise to above 65°C within seconds. That heat causes what doctors call coagulative necrosis: the cancer cells, essentially, cook and die. The surrounding healthy tissue remains unharmed because the focus is so pinpoint-accurate.
The procedure is guided in real time using either ultrasound imaging or MRI, so doctors can track exactly what is happening inside the body at every step. The patient lies on a treatment table, remains conscious throughout, and goes home the same day. No general anaesthesia. No stitches. No recovery ward.
Why This Matters So Much for Pakistan
Pakistan has one of the highest breast cancer burdens in the entire Asian continent. According to health data, breast cancer accounts for roughly one in every three cancer cases diagnosed among Pakistani women — and the numbers are rising year by year.
What makes the situation worse is not just the prevalence of the disease, but the deeply rooted cultural and social barriers that prevent women from seeking timely help. In many parts of the country — particularly in smaller cities and rural areas — fear of surgery is one of the single biggest reasons women delay or completely avoid getting diagnosed and treated.
The fear is not imagined. Surgery for breast cancer, whether a lumpectomy or a full mastectomy, carries real physical and psychological consequences. For many Pakistani women, it means disfigurement, prolonged hospital stays, the risk of surgical complications, and significant recovery time — on top of the emotional toll that any cancer diagnosis already brings.
A treatment that can destroy a tumour without cutting the body open is not just a clinical upgrade. For this population specifically, it could be the difference between a woman seeking treatment early or staying home in silence until the cancer has advanced beyond help.
What the Research Says
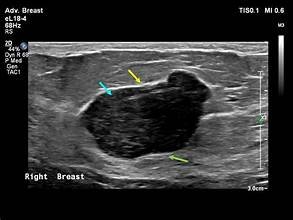
HIFU is not a fringe idea — it has been tested in clinical studies for over two decades, and results continue to build a compelling case.
A systematic review and meta-analysis published in 2024, which examined studies from PubMed and Scopus databases, found that HIFU is a “relatively safe procedure for treatment of breast cancer” and can be effective both as a standalone therapy and in combination with other treatments such as chemotherapy or radiotherapy.
An earlier landmark clinical trial conducted in China found that HIFU could induce complete coagulative necrosis of localised breast tumours, and concluded the technique was “effective, safe, and feasible” as a non-invasive external treatment. Across multiple studies, the rate of patients achieving complete tumour necrosis ranged from 17% to 100%, depending on tumour type, size, and the number of treatment sessions used.
One particularly striking case documented by the Focused Ultrasound Foundation involved a 48-year-old patient with node-positive, hormone-receptor positive breast cancer who refused surgery and underwent HIFU instead. Ten months after treatment, her breast tumour showed complete remission on ultrasound assessment, with the affected lymph node also shrinking by more than 50%.
While that is a single case and not a clinical norm, it illustrates the real potential of this technology in the right conditions.
The Science Behind the Treatment: Key Facts
For those who want to understand the basics before asking their doctor, here is a clear breakdown:
- What it targets: Localised, early-stage breast cancer tumours — typically solid masses that are clearly defined on imaging
- How it destroys cancer cells: Focused sound energy heats the tumour tissue above 65°C, causing irreversible cell death
- What it leaves intact: Surrounding healthy breast tissue, skin, and nerves — because the focus point is precise
- How long it takes: A single session typically lasts between 1 to 4 hours depending on tumour size
- Is it painful? Most patients report minimal discomfort; some centres use light sedation, though many procedures need none at all
- Who guides the treatment: A trained radiologist or oncologist using real-time ultrasound or MRI imaging
- Recovery time: Most patients resume normal activity within 24 to 48 hours
Challenges and Honest Limitations
It would be dishonest to present HIFU as a complete replacement for surgery in all cases — and specialists are careful to say so.
The therapy works best on small, localised, solid tumours that have not spread to lymph nodes or distant organs. Larger tumours, rim-enhancing lesions, and non-mass tumours show significantly lower ablation success rates. For women with advanced or metastatic breast cancer, surgery, chemotherapy, and radiation remain the standard of care.
There is also the matter of availability. HIFU equipment is expensive, requires specialised training, and is currently offered in only a handful of centres globally — mostly in China, the United Kingdom, South Korea, and a growing number of European nations. In Pakistan, widespread clinical access to this technology is still limited, though awareness among oncologists is growing.
Experts at leading cancer centres in Karachi and Lahore have noted that while the technology is promising, it needs dedicated imaging-HIFU platforms and trained bioengineering teams to deliver consistently safe results. Building that infrastructure takes time, investment, and health policy support.
What Pakistani Oncologists Are Watching

The broader medical community in Pakistan is not dismissing this development — quite the opposite. The country’s oncology landscape has been evolving, with major hospitals in urban centres increasingly looking at less invasive options to improve patient outcomes and, crucially, to reduce the fear factor that keeps women away.
Several specialists working in breast oncology have pointed to the need for government and private sector investment in newer technologies as breast cancer diagnosis rates climb. Journal of the College of Physicians and Surgeons Pakistan (JCPSP) has published multiple studies in recent years highlighting the need for improved, less invasive options in breast cancer care — especially in resource-limited settings.
The argument is straightforward: if a technology exists that can treat early-stage breast cancer without surgery, without general anaesthesia, and with minimal recovery time, then making it accessible to Pakistani patients is a public health priority — not just a medical curiosity.
Who Could Benefit From Ultrasound Therapy for Breast Cancer?
Not every patient is an immediate candidate, but the group who may benefit is significant:
- Women with early-stage, localised breast cancer — particularly those with small, well-defined solid tumours
- Patients who are medically unfit for surgery — due to heart conditions, diabetes, or other comorbidities that make anaesthesia risky
- Women who refuse surgery — for cultural, psychological, or personal reasons
- Older patients — for whom the physical stress of surgery and recovery is a serious concern
- Patients seeking breast-conserving options — who want to avoid mastectomy and its emotional and physical effects
If you or someone you know has been diagnosed with early breast cancer, asking an oncologist whether HIFU or other ablation therapies are an option is now a reasonable — and increasingly informed — question to bring to the consultation room.
What Comes Next: The Road Ahead
The global research community continues to invest in making HIFU more reliable, more widely available, and better integrated with other cancer therapies. Combination approaches — where HIFU is used together with immunotherapy or targeted drug delivery — are showing early promise in laboratory and early-stage clinical settings.
In Pakistan specifically, the hope is that increased awareness, both among patients and policymakers, will build pressure for investment in this space. Cancer treatment in the country has historically been underfunded relative to the scale of the problem. HIFU represents exactly the kind of innovation that could close the gap — provided the will and the resources follow the science.
For now, women who are diagnosed with early breast cancer in Pakistan should know this: the options available to you today are more than they were five years ago. Surgery is not always the only answer. And the sound of the future, quite literally, may be one that heals.
Final Thought!
The emergence of ultrasound therapy for breast cancer as a clinically studied, non-invasive treatment option is a genuine breakthrough — especially for a country like Pakistan where the stakes are high and the barriers to conventional treatment run deep. HIFU does not yet replace surgery for every patient, but for the right candidate, it offers something that no scalpel ever could: treatment without trauma.
As research deepens and infrastructure slowly expands, Pakistani women — and their families — deserve to have these conversations with their doctors. Awareness is the first step. Treatment is the next.
Have questions about breast cancer treatment options in Pakistan? Share this article with someone who needs to read it — and encourage the women in your life to get screened early.